TYPES OF STROKES
Exerpt: Types of Strokes, from the Gold Cross Magazine CEU Article "Recognizing And Reacting to Strokes (CVAs) And TIAs" By, Pat Leonard.
|
There are two major types of stroke: ischemic and hemorrhagic.
Ischemia - is a local decrease in blood supply due to mechanical means such as a narrowed or pluggedartery. Most often this is caused by a build-up of plaque in the arteries, a well-known condition called athersclerosis. (Photo 1) The cells within the area become ischemic, or oxygen-starved. If the condition is not reversed, the cells infarct, or die. A cerebrovascular accident occurs when a blood vessel in the brain becomes obstructed by a clot (throm-bus) which may have formed in a narrowed artery or may have originated in a different site and traveled through the blood stream to the vessels of the brain. Once obstructed, the area of brain cells becomes ischemic, and if the condition is not reversed, infarcts.
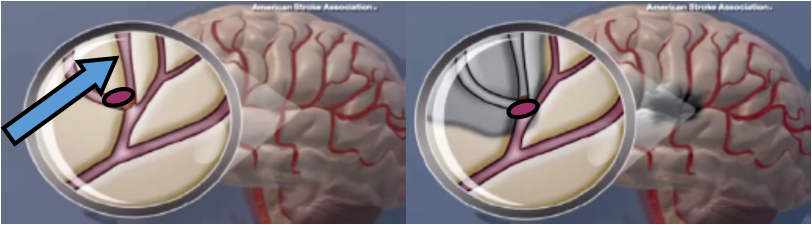
An ischemic cerebrovascular accident (CVA) occurs when blood circulation to an area of the brain is blocked (left enlargement) and vital brain tissue dies due to lack of oxygen and nutrients. The sensitive cells of the brain are permanently damaged after only four to five minutes without oxygen and glucose. When an area of the brain is deprived of these nutrients, that portion of the brain dies (right illustration) and the function it provided is altered.
A clot that originates at one site and travels to another is called an embolus. (Plural: emboli) Emboli can be fat globules, air bubbles or most commonly, bits and pieces of atherosclerotic plaque such as lipid debris that have detached from a dis-eased carotid artery or elsewhere. The bloodstream moves the embolus to another site, such as a pulmonary artery or the brain where it becomes lodged. Patients with a cardiac condition called atrial fibrillation can develop clots within the heart’s atrium which then break off and embolize into the cerebral circulation. Other patients at risk of developing thrombi and possible CVA include women who take birth control pills which makes the blood more prone to form clots. (For a list of individuals at risk for a stroke, For stroke management, “time lost is brain lost.”
Risk Factors For Stroke In addition to the factors of race and sex, individuals with the following conditions and/or lifestyle choices are at greater risk of suffering a CVA or TIA:
|
After an ischemic stroke, the amount of irreversible damage increases steadily as long as brain regions remain without sufficient blood supply. In those parts of the affected region that have no blood flow, neurons begin to die in less than ten minutes. In those areas with less than 30% of normal blood flow, neurons begin to die within an hour. In those areas with 30–40% of normal blood flow, some neurons begin to die within an hour, but others can be revived for many hours.
Hemorrhagic CVA occurs when there is a sudden rupture of a blood vessel in the brain. This may be caused by the effects of severe hypertension or drug use (e.g., cocaine), which results in bleeding within the brain. Hemorrhage may also be the result of a ruptured aneurysm, or a tear of a weakness along a wall of an artery supplying the brain. Ischemic CVAs occur far more frequently than hemorrhagic CVAs (roughly 85% of strokes are ischemic), but hemorrhagic CVAs are usually more deadly. One recent study showed that the mortality rate after a stroke (both types) was 10.5% at 30 days, 21.2% at one year, 39.8% at five years, and 58.4% at the end of follow-up. Ischemic CVAs occur far more frequently than hemorrhagic CVAs, but hemorrhagic CVAs are usually more deadly. Mortality rates after a hemorrhagic stroke were 67.9%; after an ischemic stroke the mortality rates were 57.4%.
Although it is not your job as an EMT to distinguish between types of stroke in the pre-hospital field, it is imperative that you recognize signs and symptoms of stroke, understand a CVA may be in progress and take immediate steps to maximize the functional outcome of the patient. Signs & Symptoms of Stroke
EMTs cannot assume that victims know how to recognize potential strokes. A survey by the American Heart Association found that only 55% of patients who have already had a stroke could identify even one stroke warning sign. Stroke symptoms depend on the area of the brain that is affected, which is most often the middle cerebral artery or one of its branches. Symptoms can include: numbness, weakness or paralysis on one side of the body (usually contralateral hemiplegia) or face; confusion, difficulty speaking or writing, or difficulty understanding, difficulty seeing and/or visual field defects; gait deviations. Unlike an ischemic stroke, hemorrhagic strokes can present with a sudden onset of severe (“thunder-clap”) headache. During assessment, a patient may report “the worst head-ache” of his life. The sudden increase in blood volume within the rigid skull causes a rapid increase in intracranial pressure which may result in a loss of consciousness, or even death.
At times, symptoms of CVA occur and disappear within 24 hours of onset. The EMT is dispatched for “possible CVA” and arrives to discover the patient speaking and moving about normally. This situation, though not a CVA per-se, represents a temporary obstruction of blood flow through a narrowed vessel, thus a relatively mild period of hypoxia to a part of the brain. The temporary condition is aptly termed a transient (or “passing”) ischemic attack (TIA). Patients may sometimes describe a “veil” or “window shade” partly covering the vision of one eye which resolves spontaneously after several minutes. This in fact represents the temporary blockage, or occlusion, of the retinal artery to the eye by an embolus. There may also be dizziness, imbalance and generalized weakness. Patients experiencing new onset or recurrent TIAs need medical evaluation urgently as left untreated, the condition may result in a CVA. |